
Bone wax technique for full-endoscopic lumbar laminotomy
Introduction
Full-endoscopic spine surgery (FESS) is gaining popularity; however, the control of bleeding is often problematic as it may affect the course of the surgical procedure. Typically, bipolar coagulation, application of thrombin, and other techniques are performed to control bleeding in endoscopy (1). However, they may be insufficient, especially for copious amounts of bleeding from the veins and arteries in the lamina. Under microscopic procedures, bone wax is used to stop the bleeding from the bone structures. However, it is not commonly used in endoscopy because it sticks to the endoscope working channel and lens while being conveyed to the bleeding point. We solved this problem by using a nozzle to deliver the bone wax and a drill to spread it under irrigation control. We present the following article in accordance with the CARE reporting checklist (available at https://jss.amegroups.com/article/view/10.21037/jss-22-64/rc).
Surgical technique
Representative case description
A 72-year-old female patient with L4/5 stenosis presented with right sciatic pain. An endoscopic right-side approach was performed for bilateral decompression. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from patients for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Step-by-step description of the bone wax technique (BWT)
The BWT performed during FESS for laminotomy is as follows (Figure 1 and Video 1):
- Step 1: the bone wax was loaded into the tip of the nozzle, which was 34 cm in length, with an outer diameter of 2 mm (Ethicon). Therefore, the nozzle could be inserted into a 4-mm or larger working channel of the endoscope. Irrigation was stopped to identify the bleeding point. The nozzle was placed over the bleeding point, and the wax was ejected by pushing the rod. The nozzle was removed while rotating the shaft, and the bone wax was detached and left precisely on the target.
- Step 2: the drill burr was placed on the wax, and irrigation was restarted to wash the bleeding while the bone wax was held onto the bone. The drill was driven at low speed, spreading bone wax on and around the bleeding point.
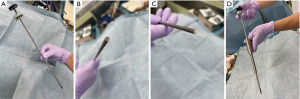
Comments
Surgical results
From Feb 2020 to Sep 2022, 121 cases of FESS for laminotomy were performed. In the initial 41 cases, BWT was not applied (non-BWT group). In the next 80 cases, BWT was applied (BWT group). These two groups were compared by χ2 analysis for sex and the event ratio of dural tear (DT) including a case of non-cerebrospinal fluid leakage with an intact arachnoid membrane. The Student’s t-test was used to analyze age and operation time. SPSS version 28 (IBM, Armonk, NY, USA) was used for the analysis. The event ratio of DT during surgery was significantly higher in the non-BWT group (29.2%) than in the BWT group (2.5%), although no significant differences in age, sex and operation time between the two groups (Table 1) were noted. In all cases, preoperative symptoms improved postoperatively.
Table 1
| Characteristics | Non-BWT (n=41) | BWT (n=80) | P value |
|---|---|---|---|
| Age (years), mean ± SD | 70.6±11.3 | 72.5±11.3 | 0.35 |
| Sex: female (%) | 30.9 | 69 | 0.61 |
| Operation time (min), mean ± SD | 173.2±53.4 | 167.7±62.1 | 0.62 |
| DT (%) | 29.2 | 2.5 | <0.001 |
BWT, bone wax technique; DT, dural tear; SD, standard deviation.
Surgical nuances of BWT
Hemostatic procedures were described systematically by Hofstetter (1). According to the paper, the bleeding point should be identified, and bipolar cautery was considered most effective when compressing the bleeding vessel with the tip and simultaneously activating coagulation. However, in the case of bone bleeding, bipolar cautery was deemed ineffective. Hofstetter’s alternative suggestion was to seal the area of bone bleeding using the diamond burr or by compression with a Kerrison rongeur. If this method failed, he suggested increasing the irrigation pressure and advancing the endoscope toward the bleeding source for better visualization of the bleeder. As a last resource, he proposed the injection of thrombin, followed by applying FLOSEAL (Baxter) into the working channel.
Initially (in the non-BWT group), we followed Hofstetter’s hemostatic step-by-step algorithm. However, we noticed that compression using the Kerrison rongeur was unable to cover some bony bleeders, whilst the injection of thrombin stopped the bleeding. However, many blood clots covered the endoscopic surgical view, which slowed down the operation. Therefore, we needed another method to achieve hemostasis. We developed BWT, which can cover various bony bleeding cases, even with issues arising from the use of the bipolar or Kerrison rongeur. We subsequently (in the BWT group) applied BWT to maintain a clean surgical field and DT diminished significantly. Care should be taken when the epidural vein is the origin of bleeding, because it is sometimes indistinguishable from the bone, especially when releasing lateral recess stenosis. In these cases, we used Bemsheets to press around the bleeding and moved to another site. For example, in case of epidural bleeders under the edge of the lateral recess, typically caused by bites with the Kerrison rongeur during the decompression of the contralateral recess (1), we placed Bemsheets on the bleeding area, moved to the approach side, and removed the side of the hypertrophied ligamentum flavum without stopping the operation. After some minutes of those procedures, we returned to the original point of Bemsheets, and removed the Bemsheets when hemostasis was achieved and continued the contralateral decompression.
Chu et al. introduced the use of bone wax in endoscopic cervical intracorporeal drilling for discectomy (2). Bone wax was smeared on the endoscopic burr as described in the paper. However, it strongly adhered to the working channel with significant wax loss, and repeated delivery was burdensome.
Our delivery method using a nozzle solved this problem, providing a smooth and significant hemostatic effect, and notably improved the endoscopic surgical view, thereby allowing safe and effective procedures.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at https://jss.amegroups.com/article/view/10.21037/jss-22-64/rc
Peer Review File: Available at https://jss.amegroups.com/article/view/10.21037/jss-22-64/prf
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jss.amegroups.com/article/view/10.21037/jss-22-64/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from patients for publication of this case report and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Hofstetter CP. Principles of Full-Endoscopic Surgical Technique. In: Hofstetter CP, Ruetten S, Zhou Y, et al, editors. Atlas of Full-Endoscopic Spine Surgery. New York, NY, USA: Thieme, 2020:36-8.
- Chu L, Yang JS, Yu KX, et al. Usage of Bone Wax to Facilitate Percutaneous Endoscopic Cervical Discectomy Via Anterior Transcorporeal Approach for Cervical Intervertebral Disc Herniation. World Neurosurg 2018;118:102-8. [Crossref] [PubMed]


