
Differences in primary and revision deformity surgeries: following 1,063 primary thoracolumbar adult spinal deformity fusions over time
Introduction
Adult spinal deformity (ASD) is a common pathology that can lead to decreased quality of life, increased pain, physical limitations, and dissatisfaction with self-image (1,2). It is a complex disease that may result from developmental deformities obtained at a young age or arise de novo later in life. Degenerative changes of the spine as well as trauma and tumors are amongst other etiologies that can lead to spinal deformity (3). As such, the treatment of ASD can vary widely and may become quite complex in order to address both the underlying issue as well as the deformity itself.
The initial management of ASD often consists of non-operative treatment in the form of pain reduction and improvement of physical function in the form of physical therapy and exercise, the efficacy of such interventions is not well supported in the literature (4,5). As such, ASD often requires surgical treatment, especially in patients who have progression of their deformities, neural compromise, intolerable pain, and severe limitations in physical function (6-8). However, as with any treatment, surgery for ASD comes with its own risks, including neurological and cardiovascular complications (9). Furthermore, operative treatment also exposes patients to the possible need for revision surgery (10).
Revisions for ASD are reported at rates as high as 32% (11). These surgeries are of the utmost importance as rates of ASD surgeries increase on an aging population (12). There is a conflict in the literature, however, over complication risks and protocol differences in primary versus revision surgeries. Although common clinical sense would predict higher complication rates in revision surgeries, the literature has shown no complication differences between either patient group (13). However, these studies may suffer from small sample sizes, as protracted follow-up on ASD patients is sparse in the literature.
The goal of the current study was to use a large state-wide patient database with long-term patient tracking to follow primary ASD fusion patients and their respective revisions over many years. While operative treatment for ASD has been thoroughly studied, ASD revision rates and long-term follow-up have only been done so in smaller patient samples (12,14,15).
Methods
Data source
The State Inpatient Database of New York (NYSID) was created by the Healthcare Cost and Utilization Project sponsored by the Agency for Healthcare Research and Quality. This database contains patient information derived from billing data, and includes patients covered by Medicare, Medicaid, and Private Insurance. The NYSID includes over 500 clinical and nonclinical data elements: diagnoses, procedures, patient demographics, charges, length of stay (LOS), and hospital characteristics. Diagnosis and procedural codes are given using the International Classification of Diseases-Ninth Revision—clinical modification (ICD-9-CM). Unique patient identifiers allow linkage of data from multiple years and identification of repeat hospitalizations.
Study population
This study isolated patients over the age of 18 on NYSID from the years 2009–2013 undergoing 5+ levels of thoracolumbar spinal fusion (ICD-9-CM codes 81.xx) for a primary diagnosis of scoliosis (ICD-9-CM codes 737.xx). Patients meeting the above inclusion criteria without any prior surgeries on the database and undergoing primary fusion were identified as the ‘Primary’ fusion group. Using follow-up data time-points, additional fusions performed on the lumbar spine were identified as ‘Revision’ procedures.
Analysis
Primary analysis compared demographic, perioperative outcomes, procedural differences, and complications between revision and primary procedures using t-tests for continuous variables and chi-squared tests for categorical variables. Demographic data compared included: age, Charlson comorbidity index (CCI) score, gender, race, admission type (emergency, urgent, or elective), and weekend admission status. Perioperative outcomes included: LOS, total charges, and discharge disposition (routine, short term hospital, another facility, or home health care). Procedural information queried were: levels fused, interbody support (y/n), bone morphogenetic protein (BMP) (y/n), decompression (y/n), and approach. Finally, complications were available: dysphagia, neurological (any central nervous system, cerebrovascular infarction or hemorrhage, or other unclassified), cardiovascular, PVD, respiratory (including pneumonia and other ventilator associated complications not elsewhere classified), gastrointestinal, urological, and device-related (mechanical device complications and those requiring removal of hardware) in nature as well as shock (any shock during or resulting from procedure), hematoma formation, accidental surgical laceration, infection (in-hospital), anemia, ARDS, PE, and DVT.
Multivariate regression controlling for age, sex, number of levels fused, and CCI score then compared primary and revision surgeries based on the same factors. A sub-analysis analyzed predictors in primary patients as predictive of sustaining a revision using the same procedures of t-tests, chi-squared tests, and multivariate regression. SPSS version 21.0 was used for all statistical testing. Significance was set at P<0.05.
Results
Overview
A total of 1,063 patients who underwent corrective surgery for ASD were identified on the NYSID database (primary group). Among them, 123 (11.6%) underwent a subsequent additional re-fusion procedure with an average of 328 days in between fusions (revision group). The most frequent revision etiologies were implant failure (43.1%), acquired kyphosis (24.4%), enduring scoliosis (14.6%), fracture (8.1%), and infection (4.1%). Demographic information comparing primary and revision procedures is available in Table 1. Revisions were older (47.63 vs. 61.43 years; P<0.001), had a higher proportion female (69.0% vs. 80.5%; P=0.008), and were more frequently an emergency admission (2.4% vs. 13.8%; P<0.001). However, both Primary and Revision groups had similar comorbidity burden (1.23 vs. 1.11; P=0.321). The most common cause for revision surgery was implant failure (43.09%) followed by acquired kyphosis (24.39%) and enduring scoliosis (14.63%).
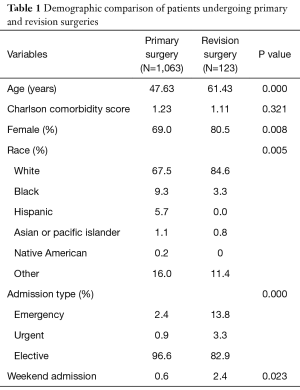
Full table
Procedures in revisions
In comparing procedural averages, there was no significant difference between surgical groups when comparing rates of decompressions (P=0.829), anterior approach (P=0.783), posterior approach (P=0.721), or combined approach (P=0.831) (Table 2). The mean number of levels fused was significantly less in revision surgeries than in primary surgeries (7.1 vs. 7.4, respectively; P=0.013). Revision surgeries were found to utilize interbody devices significantly less (29.3% vs. 40.1%; P=0.020) while having a higher utilization of BMP (43.9% vs. 32.1%; P=0.008).
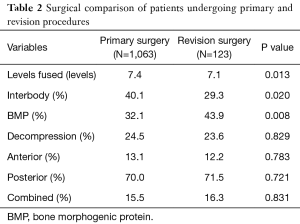
Full table
Outcomes in revisions
Table 3 details perioperative outcomes in either group. There was no difference between Primary and Revision surgeries in LOS (7.2 vs. 8.1 days; P=0.110). However, revision procedures had an average ‘total charge’ of ~$27,000 less (P=0.013). Both primary and revision surgeries also had similar discharge dispositions in terms of undergoing either a routine discharge or to another facility or even to home with home health care (P=0.159).
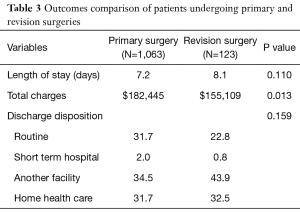
Full table
Complications in revisions
The risk of infection was found to be higher in revision surgeries (OR: 3.49, 95% CI: 0.86–14.19; P=0.041). Complications, overall, were similar between the two groups (OR: 0.81, 95% CI: 0.45–1.49; P=0.697) (Table 4).
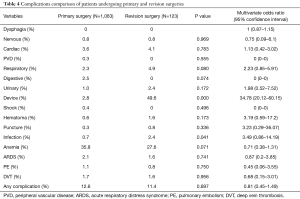
Full table
Risk of revision
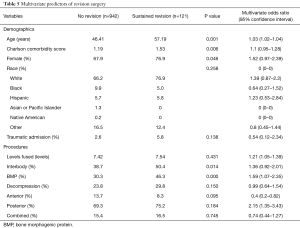
Table 5 describes predictors for requiring revision surgery. Patients that were older had slightly increased risk of undergoing a revision surgery (OR: 1.03, 95% CI: 1.02–1.04; P=0.001). No other demographic parameters revealed any significance in terms of increased risk for undergoing revision surgery. The only surgical variable associated with an increased risk of undergoing revision was BMP usage in the primary procedure (OR: 1.59, 95% CI: 1.07–2.35; P<0.001).
Full table
Discussion
With the prevalence of adult scoliosis estimated to be as high as 32% in the general population and even higher amongst the older population, the need for advancements in evidence-based medicine and management are crucial (2,11). Rates and characteristics of revision surgeries for ASD have been discussed in the literature but not as thoroughly as those for primary surgeries have, which may be due in part to smaller patient populations. As such, we analyzed a large inpatient statewide database to assess differences between primary and revision surgeries for ASD. In addition, we also aimed to describe predictors for revision surgeries based on both patient and primary surgery factors.
In our study population, we found a revision rate of 11.6%, which is in line with those from other studies. Studies have found revision rates for ASD ranging from 9.0% up to as high as 47% (16-23). We found that that revision surgeries were much more likely to be performed emergently than primary surgeries, which also accounts for the increased rate of emergent admissions in revision surgeries. Zhu et al. found that in patients who required emergent revision surgery for ASD, hardware breakage was the most common reason for revision, with over a third (37.1%) of cases having this diagnosis (24). This is in agreement with our findings in that 43.09% of revisions were accounted for by implant failure. Furthermore, proximal junctional kyphosis may account for a large percentage of these emergent cases, as we found about a quarter of revision surgeries were performed for acquired kyphosis. The resulting junctional disorder can lead to cord compression, especially in those with osteoporosis, necessitating the need for emergent correction (25).
We found that revision surgery patients were on average 13.8 years older in age than primary surgery patients. Older patients tend to have more comorbidities, which predisposes them to greater risk for post-operative complications (2,24,26,27). This greater risk may also lead to more indications for need for revision surgeries. We did not find an increased risk of undergoing revision surgery in female patients even though a significantly higher percentage of revision patients were female as compared to the primary cohort. This is in contrast to some other studies that found no difference in sex between those underwent revision and those who did not (12,22,23). Given the higher rate of osteoporosis, a higher revision rate in women may indicate that osteoporosis plays an important role in influencing the need for reoperation. Osteoporosis may contribute to the increase in revision rates due to non-union secondary to poor bone stock (28).
Our analysis found an increased rate of infection in revision surgeries as compared to primary surgeries. However, this result proved to be statistically non-significant when a multivariate analysis was performed. This is in contrast to other studies that have found increased rates of infection in revision surgeries (29,30). When other medical complications in primary and revision surgeries were analyzed, there were no statistically significant differences in any of the medical complications or total complication rates. This is in agreement with the study performed by Cho et al. that found similar complication rates between primary and revision surgeries in patients 40 years or older (12). Given that those who underwent revision were significantly older and the generally greater comorbidity burden in older patients, it may be unexpected that complication rates remained similar between primary and revision surgeries (2). However, the lack of difference may be attributed to improvements in anesthetic and surgical techniques as well as careful choice of patients where the benefits of surgical intervention outweighs potential risks (31,32). This may also explain why we found no significant difference between CCI in primary versus revision surgeries.
In terms of surgical factors, we identified no significant differences besides interbody and BMP usage, with interbody usage being significantly decreased in revision surgeries and BMP increasing in revision surgeries. This increase in BMP usage may be due to the increased rates of traumatic admissions. Studies have found that pseudarthrosis is one of the more common reasons for having to undergo a revision surgery (22,24). As such, increases in BMP usage in revision surgeries may be attributed to surgeons aiming to achieve better fusions (33).
When we compared patients who underwent revision with those who did not, we found that greater age and BMP usage were predictive of undergoing a revision surgery. BMP is often used the setting of achieving greater bony fusion. As such, surgeons may have a selective bias in which patients they choose to utilize BMP. Clinicians may be more likely to utilize BMP in those more prone to pseudarthrosis, which includes those with greater comorbidities such as osteoporosis (34). Moreover, those who had BMP usage in their primary surgeries may have undergone more complex and higher risk deformity corrections, which in itself may be a risk factor for revisions (35). These findings are in contrast with Puvanesarajah et al. who found that BMP usage is associated with a decreased risk for revision surgery (20).
We appreciated limitations to our study, including the use of a state-wide database and its retrospective nature. While such large databases offer large patient samples, they often lack granularity in terms of their data. Furthermore, given the nature of a large database that encompasses multiple health care centers, there may be variability in healthcare protocols, however, this may represent the overall diversity of surgical practice.
Conclusions
In total, 10% of ASD patients undergoing scoliosis correction required revision. The most frequent causes for revision were: implant failure, iatrogenic kyphosis, and enduring scoliosis. Revision surgeries had higher infection incidence, but no other complication rate differences.
Acknowledgements
None.
Footnote
Conflicts of Interest: Dr. PG Passias discloses consulting agreements with Medicrea, Zimmer Biomet, and Spinewave, as well as scientific advisory board membership with Allosource. The other authors have no conflicts of interest to declare.
Ethical Statement: IRB approval was not necessary for this study, as it uses nationally available, de-identified data.
References
- Bess S, Line B, Fu KM, et al. The Health Impact of Symptomatic Adult Spinal Deformity: Comparison of Deformity Types to United States Population Norms and Chronic Diseases. Spine (Phila Pa 1976) 2016;41:224-33. [Crossref] [PubMed]
- Ames CP, Scheer JK, Lafage V, et al. Adult Spinal Deformity: Epidemiology, Health Impact, Evaluation, and Management. Spine Deform 2016;4:310-22. [Crossref] [PubMed]
- Grubb SA, Lipscomb HJ, Coonrad RW. Degenerative adult onset scoliosis. Spine (Phila Pa 1976) 1988;13:241-5. [Crossref] [PubMed]
- Everett CR, Patel RK. A systematic literature review of nonsurgical treatment in adult scoliosis. Spine (Phila Pa 1976) 2007;32:S130-4. [Crossref] [PubMed]
- Glassman SD, Berven S, Kostuik J, et al. Nonsurgical resource utilization in adult spinal deformity. Spine (Phila Pa 1976) 2006;31:941-7. [Crossref] [PubMed]
- Smith JS, Shaffrey CI, Berven S, et al. Operative versus nonoperative treatment of leg pain in adults with scoliosis: a retrospective review of a prospective multicenter database with two-year follow-up. Spine (Phila Pa 1976) 2009;34:1693-8. [Crossref] [PubMed]
- Smith JS, Fu K-M, Urban P, et al. Neurological symptoms and deficits in adults with scoliosis who present to a surgical clinic: incidence and association with the choice of operative versus nonoperative management. J Neurosurg Spine 2008;9:326-31. [Crossref] [PubMed]
- Liu S, Schwab F, Smith JS, et al. Likelihood of reaching minimal clinically important difference in adult spinal deformity: a comparison of operative and nonoperative treatment. Ochsner J 2014;14:67-77. [PubMed]
- Smith JS, Shaffrey CI, Glassman SD, et al. Risk-benefit assessment of surgery for adult scoliosis: an analysis based on patient age. Spine (Phila Pa 1976) 2011;36:817-24. [Crossref] [PubMed]
- Acosta FL, McClendon J, O’Shaughnessy BA, et al. Morbidity and mortality after spinal deformity surgery in patients 75 years and older: complications and predictive factors. J Neurosurg Spine 2011;15:667-74. [Crossref] [PubMed]
- Schwab F, Dubey A, Gamez L, et al. Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population. Spine (Phila Pa 1976) 2005;30:1082-5. [Crossref] [PubMed]
- Cho SK, Bridwell KH, Lenke LG, et al. Comparative Analysis of Clinical Outcome and Complications in Primary Versus Revision Adult Scoliosis Surgery. Spine (Phila Pa 1976) 2012;37:393-401. [Crossref] [PubMed]
- Lapp MA, Bridwell KH, Lenke LG, et al. Long-term complications in adult spinal deformity patients having combined surgery a comparison of primary to revision patients. Spine (Phila Pa 1976) 2001;26:973-83. [Crossref] [PubMed]
- Yadla S, Maltenfort MG, Ratliff JK, et al. Adult scoliosis surgery outcomes: a systematic review. Neurosurg Focus 2010;28. [Crossref] [PubMed]
- Charosky S, Guigui P, Blamoutier A, et al. Complications and risk factors of primary adult scoliosis surgery: a multicenter study of 306 patients. Spine (Phila Pa 1976) 2012;37:693-700. [Crossref] [PubMed]
- Diebo BG, Passias PG, Marascalchi BJ, et al. Primary Versus Revision Surgery in the Setting of Adult Spinal Deformity: A Nationwide Study on 10,912 Patients. Spine (Phila Pa 1976) 2015;40:1674-80. [Crossref] [PubMed]
- Hallager DW, Karstensen S, Bukhari N, et al. Radiographic Predictors for Mechanical Failure following Adult Spinal Deformity Surgery - A Retrospective Cohort Study in 138 Patients. Spine (Phila Pa 1976) 2017;42:E855-63. [Crossref] [PubMed]
- O’Shaughnessy BA, Bridwell KH, Lenke LG, et al. Does a long-fusion “T3-sacrum” portend a worse outcome than a short-fusion “T10-sacrum” in primary surgery for adult scoliosis? Spine (Phila Pa 1976) 2012;37:884-90. [Crossref] [PubMed]
- Scheer JK, Lafage V, Smith JS, et al. Maintenance of radiographic correction at 2 years following lumbar pedicle subtraction osteotomy is superior with upper thoracic compared with thoracolumbar junction upper instrumented vertebra. Eur Spine J 2015;24 Suppl 1:S121-30. [Crossref] [PubMed]
- Puvanesarajah V, Shen FH, Cancienne JM, et al. Risk factors for revision surgery following primary adult spinal deformity surgery in patients 65 years and older. J Neurosurg Spine 2016;25:486-93. [Crossref] [PubMed]
- Paul JC, Lonner BS, Goz V, et al. Complication rates are reduced for revision adult spine deformity surgery among high-volume hospitals and surgeons. Spine J 2015;15:1963-72. [Crossref] [PubMed]
- Pichelmann MA, Lenke LG, Bridwell KH, et al. Revision rates following primary adult spinal deformity surgery: six hundred forty-three consecutive patients followed-up to twenty-two years postoperative. Spine (Phila Pa 1976) 2010;35:219-26. [Crossref] [PubMed]
- Glassman SD, Dimar II JR, Carreon LY. Revision Rate After Adult Deformity Surgery. Spine Deform 2015;3:199-203. [Crossref] [PubMed]
- Zhu F, Bao H, Liu Z, et al. Unanticipated Revision Surgery in Adult Spinal Deformity. Spine (Phila Pa 1976) 2014;39:S174-82. [Crossref] [PubMed]
- Arlet V, Aebi M. Junctional spinal disorders in operated adult spinal deformities: present understanding and future perspectives. Eur Spine J 2013;22 Suppl 2:S276-95. [Crossref]
- Worley N, Marascalchi B, Jalai CM, et al. Predictors of inpatient morbidity and mortality in adult spinal deformity surgery. Eur Spine J 2016;25:819-27. [Crossref] [PubMed]
- Klineberg EO, Passias PG, Jalai CM, et al. Predicting Extended Length of Hospital Stay in an Adult Spinal Deformity Surgical Population. Spine (Phila Pa 1976) 2016;41:E798-805. [Crossref] [PubMed]
- Park SB, Chung CK. Strategies of Spinal Fusion on Osteoporotic Spine. J Korean Neurosurg Soc 2011;49:317-22. [Crossref] [PubMed]
- Eichholz KM, Ryken TC. Complications of revision spinal surgery. Neurosurg Focus 2003;15. [Crossref] [PubMed]
- Smith JS, Shaffrey CI, Sansur CA, et al. Rates of infection after spine surgery based on 108,419 procedures: a report from the Scoliosis Research Society Morbidity and Mortality Committee. Spine (Phila Pa 1976) 2011;36:556-63. [Crossref] [PubMed]
- Cloyd JM, Acosta FL, Ames CP. Complications and outcomes of lumbar spine surgery in elderly people: a review of the literature. J Am Geriatr Soc 2008;56:1318-27. [Crossref] [PubMed]
- Wang MY, Widi G, Levi AD. The safety profile of lumbar spinal surgery in elderly patients 85 years and older. Neurosurg Focus 2015;39. [Crossref] [PubMed]
- Etminan M, Girardi FP, Khan SN, et al. Revision strategies for lumbar pseudarthrosis. Orthop Clin North Am 2002;33:381-92. [Crossref]
- Leven D, Cho SK. Pseudarthrosis of the Cervical Spine: Risk Factors, Diagnosis and Management. Asian Spine J 2016;10:776-86. [Crossref] [PubMed]
- Poorman GW, Jalai CM, Boniello A, et al. Bone morphogenetic protein in adult spinal deformity surgery: a meta-analysis. Eur Spine J 2017;26:2094-102. [Crossref] [PubMed]


